GLP-1 Cost & Access
Summary: Brand GLP-1s in the United States carry list prices of roughly $968 to $1,349 a month, but almost nobody actually pays that. Manufacturer cash channels (NovoCare Pharmacy at $499 a month for all Wegovy doses, LillyDirect Zepbound vials starting at $349 and dropping to $299 in the Self-Pay Journey Program), expanded Medicare access through the new GLP-1 Bridge program at a $50 copay starting July 2026, generic liraglutide from Hikma in the $250 to $500 range, and licensed 503A compounding pharmacies billing $99 to $400 a month have all moved real out-of-pocket prices well below list. This guide walks through every legitimate path, what each one actually costs in 2026, who qualifies, and how to assemble the cheapest legal route to your prescription. [1][2][3][4][5]
This content is for informational purposes only and is not medical advice. Always consult a qualified healthcare provider before starting, changing, or stopping any medication.
What GLP-1s actually cost at the pharmacy counter
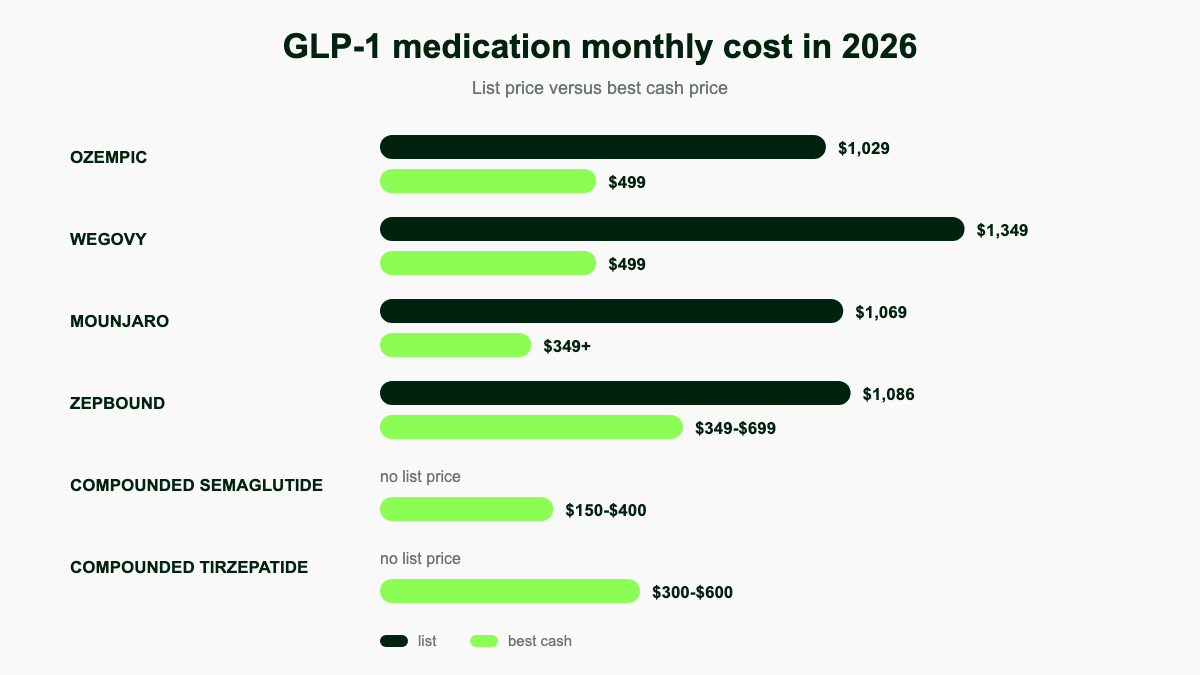
The headline list prices for GLP-1 medications in the United States are some of the highest sticker prices in retail medicine. Without insurance, expect a single month of brand therapy to fall in the four-figure range at most chain pharmacies, with the biggest gap of any major drug class between the published list price and the price a determined cash payer can actually find. [1][2][3]
The table below shows the 2026 cash list price for each major brand GLP-1 along with the lowest legitimate direct-from-manufacturer cash channel for that product. The list price is what an uninsured patient walking into a CVS or Walgreens with no card and no program is quoted. The right-hand column is what the same patient pays if they call the manufacturer pharmacy or use the manufacturer self-pay program. The difference is rarely less than 50 percent and is sometimes 75 percent. [1][2][6]
| Medication | Maker | Indication | Cash list price (per month) | Lowest direct-from-maker cash price |
|---|---|---|---|---|
| Ozempic (semaglutide) | Novo Nordisk | Type 2 diabetes | $997.58 (all strengths) [1][6] | $199 first 2 fills 0.25 / 0.5 mg via NovoCare; then $349 for 0.25 / 0.5 / 1 mg, $499 for 2 mg [6] |
| Wegovy (semaglutide) | Novo Nordisk | Chronic weight management | $1,349 [1][2] | $499 / month all doses via NovoCare Pharmacy [2][7] |
| Wegovy oral (semaglutide tablets) | Novo Nordisk | Chronic weight management | ~$1,349 (estimated, follows injection list) [7] | $149 for 1.5 mg and 4 mg via NovoCare; $199 to $399 for higher doses [7] |
| Mounjaro (tirzepatide) | Eli Lilly | Type 2 diabetes | $1,069 [3][8] | $25 with savings card if commercially insured; $573 cash savings offer [8] |
| Zepbound pens (tirzepatide) | Eli Lilly | Chronic weight management | $1,086 [3][9] | $25 with savings card if commercially insured; $650 cash savings offer [9] |
| Zepbound vials (LillyDirect) | Eli Lilly | Chronic weight management | ~$1,086 retail equivalent [3][4] | Standard: $349 (2.5 mg), $499 (5 mg), $599 (7.5 mg), $699 (10 mg), $849 (12.5 mg), $1,049 (15 mg). Self-Pay Journey Program: $299 (2.5 mg), $399 (5 mg), $449 all higher doses [4][9] |
| Rybelsus (oral semaglutide) | Novo Nordisk | Type 2 diabetes | $997.58 (3, 7, 14 mg) [10] | List drops to $675 January 2027 per Novo announcement; manufacturer savings card to $25 with insurance [10] |
| Saxenda (liraglutide) | Novo Nordisk | Chronic weight management | ~$1,349 [11] | ~$372 with GoodRx; limited manufacturer savings [11] |
| Victoza (liraglutide) | Novo Nordisk | Type 2 diabetes | $544 (2 pens) to $815 (3 pens) [11] | Generic liraglutide ~$250 to $500 / month [11] |
| Generic liraglutide (Hikma, Meitheal) | Hikma, Meitheal | Type 2 diabetes (and Saxenda equivalent dosing) | ~$410 (2 pens) to $750 (3 pens) [11] | Cash $250 to $500 / month at participating pharmacies [11] |
| Compounded semaglutide | 503A pharmacies via telehealth | Off-label / non-FDA-approved formulation | $99 to $400 [3][12] | Varies by clinic, dose, and titration plan |
| Compounded tirzepatide | 503A pharmacies via telehealth | Off-label / non-FDA-approved formulation | $125 to $600 [3][12] | Varies by clinic, dose, and titration plan |
Two patterns explain almost everything else on this page. First, the brand list price is a starting point for negotiation, not what insured Americans pay at the counter and not what informed cash payers pay either. Second, the gap between that list price and what the manufacturers will sell directly to a self-pay patient is now enormous, because Novo Nordisk and Eli Lilly are competing both with each other and with compounding pharmacies for the same uninsured demand. That competitive pressure is the single most important development in GLP-1 affordability since the drugs launched. [2][4][7]
Why US prices are so high in the first place
To choose the right access path, it helps to understand why the headline numbers are so high. US drug pricing is the product of a few interacting forces specific to this country. [13][14]
- Patent protection and exclusivity. Novo Nordisk's core semaglutide composition patents run out in late 2031 in the United States, with secondary patents extending parts of the protection. Eli Lilly's tirzepatide composition is protected into the mid-2030s. Until those expire, no generic injectable semaglutide or tirzepatide can be sold in the US. [13]
- Limited Medicare price negotiation, historically. Until the Inflation Reduction Act of 2022, Medicare was statutorily prohibited from negotiating drug prices. The first round of Medicare-negotiated prices took effect January 2026 and included Novo Nordisk's semaglutide products (Ozempic, Wegovy, Rybelsus) at a maximum fair price of roughly $245 per 30-day equivalent. Tirzepatide is a candidate for selection in later negotiation cycles. [14][15]
- PBM rebate dynamics. Pharmacy benefit managers extract large confidential rebates off list price in exchange for formulary placement, which keeps the public list price high while the actual net price paid by insurers is much lower. The cash payer at the counter has no access to that rebate.
- No reference pricing. Most peer countries set drug prices through some form of reference to clinical value or to international benchmarks. The US has not done this for prescription drugs at the federal level until the IRA negotiations and the 2025 Most-Favored-Nation framework agreements with Lilly and Novo. [16]
A widely cited Yale and King's College analysis put the production cost of semaglutide at roughly $5 per month, against a US list of more than $1,000. That gap is a margin gap, not a manufacturing-cost gap, which is why the manufacturers can profitably sell directly to cash payers at $499 once the rebate-driven pricing logic is bypassed. [13][17]
Insurance coverage by scenario
What you pay depends almost entirely on who your insurer is and what the prescription is for. The clearest split is between the diabetes indication (broad coverage) and the weight management indication (sparse and tightening coverage). [18][19]
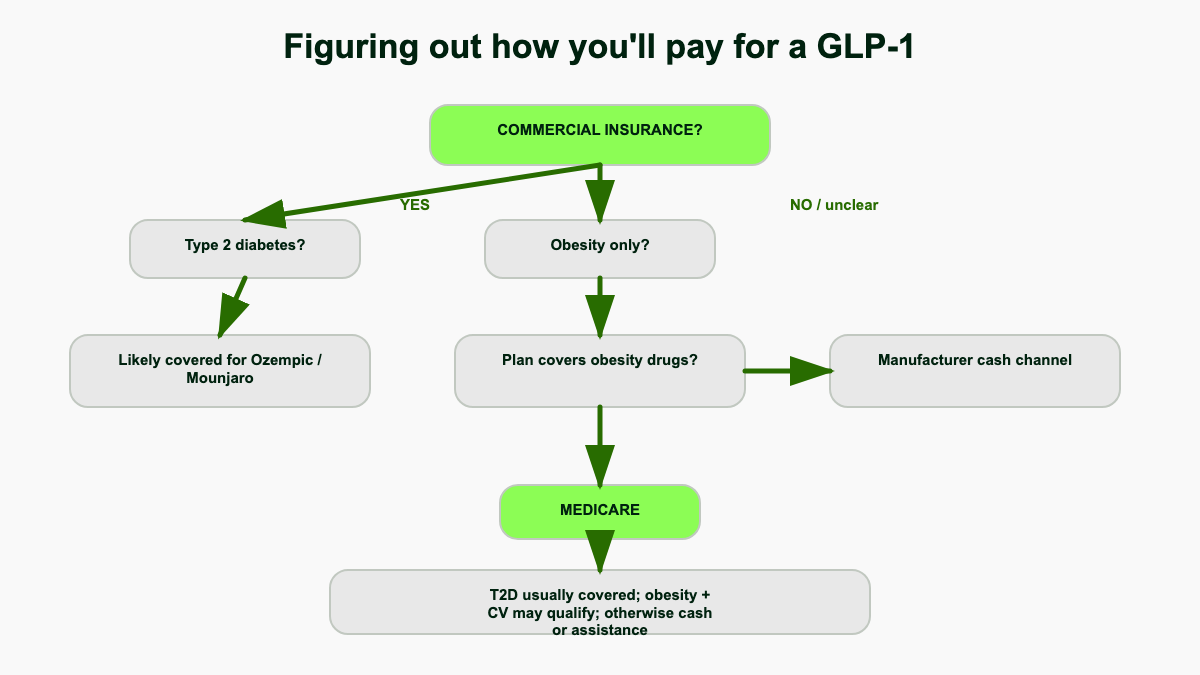
Commercial (employer or marketplace) plans
If you have type 2 diabetes, commercial coverage of Ozempic, Mounjaro, Trulicity, and Rybelsus is the default in 2026. Most large employer plans, BlueCross BlueShield products, Aetna, Cigna, UnitedHealthcare, and Kaiser cover at least one of these on their formulary, almost always with prior authorization that requires a documented diabetes diagnosis (usually an A1c above 6.5 percent or a clinician attestation). Step therapy is common, requiring a trial of metformin first, sometimes also a sulfonylurea or DPP-4 inhibitor. Copays for insured diabetes patients commonly land between $25 and $100 per month, with the manufacturer savings card pulling that to $25 in many cases. [8][18]
If you want a GLP-1 for weight management without diabetes, coverage is sparse and getting sparser. As of 2026, 8.5 percent of commercially insured people have no coverage at all for any GIP / GLP-1 agonist prescribed for weight loss. The number of people whose plan does not cover Wegovy grew 42 percent between 2025 and 2026, leaving over 41 million people with no Wegovy coverage. The number with no Zepbound coverage grew 12 percent, leaving over 109 million people with no Zepbound coverage. Where coverage exists, more than 88 percent of plans require prior authorization. [18]
| Coverage element | Diabetes (Ozempic, Mounjaro) | Weight management (Wegovy, Zepbound) |
|---|---|---|
| Plan covers it on formulary | Most commercial plans | Roughly 35 to 65 percent of commercial plans depending on employer [18] |
| Prior authorization required | Common (documented T2D) | Almost always required [18] |
| BMI threshold for PA | n/a | BMI 30 or BMI 27 with comorbidity [18][19] |
| Lifestyle program required first | Sometimes | Often 3 to 6 months documented [19] |
| Step therapy | Metformin first is common | Some plans require Contrave or Saxenda first [19] |
| Reauthorization | Annual labs | Often 5 percent body weight loss in 6 to 12 months [19] |
| Typical patient copay with coverage | $25 to $100 / month | $25 to $150 / month, with manufacturer card often $25 |
If your plan covers the drug at all, always layer the manufacturer savings card on top before paying. The card is what gets a Wegovy patient with covered access from a $150 plan copay down to $25.
Medicare
Medicare coverage of GLP-1s changed substantially in 2026. The starting point is statute: Medicare Part D is prohibited from covering drugs used solely for weight loss, a restriction that dates to the Medicare Modernization Act of 2003. That rule still applies, but two parallel paths now expand access. [20][21]
Coverage by indication: Medicare Part D plans have always covered Ozempic, Mounjaro, Trulicity, Rybelsus, and Victoza for type 2 diabetes when prescribed appropriately. Wegovy picked up a Medicare carve-out in 2024 for adults with established cardiovascular disease who also have overweight or obesity, after the FDA expanded its label to reduce major adverse cardiovascular events based on the SELECT trial. Zepbound picked up a parallel carve-out in 2024 for adults with moderate-to-severe obstructive sleep apnea and obesity, based on the SURMOUNT-OSA trial. In both cases the patient must have the qualifying comorbidity, not just obesity, and the prescriber must document it. [20]
Medicare GLP-1 Bridge program: starting July 1, 2026 and running through December 31, 2027, CMS will run the Medicare GLP-1 Bridge demonstration. Eligible Part D beneficiaries with obesity (BMI 30 or above) and at least one comorbidity can access Wegovy, the Zepbound KwikPen, and a future Lilly product called Foundayo at a $50 monthly copay. The $50 copay is possible because Novo Nordisk and Lilly agreed to a $245 net price per month with Medicare under the broader White House Most-Favored-Nation pricing deals announced in November 2025. The Bridge program does not cover patients whose GLP-1 is already coverable under existing Part D rules, so a patient who qualifies for Zepbound for sleep apnea uses standard Part D rather than the Bridge. [4][16][22]
Inflation Reduction Act $2,100 cap: Part D out-of-pocket spending is capped at $2,100 for 2026 (up from $2,000 in 2025), which means even a high-cost GLP-1 paid through Part D cannot exceed that annual ceiling for the patient. The $35-per-month insulin cap is a separate provision that does not apply to GLP-1s. [15]
Medicaid
Medicaid coverage of GLP-1s is fragmented and changing fast. As of January 2026, only 13 state Medicaid fee-for-service programs cover GLP-1s for obesity treatment. The states with obesity coverage include Delaware, Kansas, Michigan (now restricted to BMI 40 or higher as of January 1, 2026), Minnesota, Mississippi, Missouri, Tennessee, Utah, Virginia, Wisconsin, and three additional states. [23][24]
Four states (California, New Hampshire, Pennsylvania, and South Carolina) eliminated Medicaid GLP-1 coverage for obesity in 2025. North Carolina temporarily dropped coverage in October 2025 and reinstated it in December. Coverage for diabetes remains universal across all 50 state Medicaid programs because GLP-1s are first-line therapies for type 2 diabetes per ADA standards. [23][24]
The CMS BALANCE Model, launching in Medicaid as early as May 2026, lets states opt in to negotiated GLP-1 pricing tied to a comprehensive obesity care framework. Participation is voluntary for both states and manufacturers. State coverage decisions are driven primarily by budget pressure rather than clinical evidence. [23][24][25]
| Medicaid status (January 2026) | Examples | Notes |
|---|---|---|
| Covers for diabetes | All 50 states | Prior auth and step therapy common [23] |
| Covers for obesity (any criteria) | 13 states including DE, KS, MI, MN, MS, MO, TN, UT, VA, WI | Subject to PA and BMI thresholds [23][24] |
| Recently dropped obesity coverage | CA, NH, PA, SC | Cost cited as primary driver [24] |
| Restricted obesity coverage | Michigan (BMI 40+ effective Jan 2026) | Stricter PA criteria added [24] |
| Joining BALANCE Model | Opt-in starting May 2026 | Coverage depends on state and manufacturer participation [25] |
VA and TRICARE
The Department of Veterans Affairs covers semaglutide as a non-formulary medication with criteria for use, meaning it requires prior authorization through the VA pharmacy and is generally prescribed after first-line options for the relevant indication. VA clinics that have piloted GLP-1 prescribing for veterans with obesity have reported strong outcomes. [26]
TRICARE Prime and TRICARE Select cover Wegovy, Zepbound, and Saxenda for weight management with prior authorization, but TRICARE For Life dropped weight-loss drug coverage as of August 31, 2025. The fiscal 2026 National Defense Authorization Act expanded TRICARE coverage for weight-loss drugs when prescribed by a network provider as part of a comprehensive treatment plan. For diabetes, TRICARE covers Ozempic, Mounjaro, Trulicity, and Victoza with prior authorization. [27]
Manufacturer savings cards (commercial insurance only)
Both manufacturers run copay assistance for their flagship GLP-1s. These cards are designed for patients who already have private insurance covering the drug, and they reduce the patient's out-of-pocket share. They are not available to anyone with Medicare, Medicaid, TRICARE, the VA, or other government coverage; using one while enrolled in a government plan can violate the federal anti-kickback statute and program rules. [6][8][9]
- Ozempic Savings Card: commercially insured patients can pay as little as $25 for a 1-month or 3-month supply, with a maximum savings of up to $150 per month. The card is valid for up to 48 months from first activation. [6]
- Wegovy Savings Offer: commercially insured patients with coverage can pay as little as $0 per 28-day supply when their plan covers the drug, with a monthly cap on what the savings offer pays toward the bill. Patients without coverage are routed to NovoCare Pharmacy at $499 cash. [7]
- Mounjaro Savings Card: commercially insured patients with coverage can pay as little as $25 for up to a 3-month supply. Patients with commercial insurance that does not cover Mounjaro can pay $573 per month under a separate offer. [8]
- Zepbound Savings Card: commercially insured patients with coverage can pay as little as $25 per month, and patients with commercial insurance that does not cover Zepbound can pay $650 per month for pens or use LillyDirect for cheaper vials. [9]
- Rybelsus Savings Card: commercially insured patients can pay as little as $25 per 30-, 60-, or 90-day supply, with a maximum savings of $100 per 30-day supply. [10]
- Saxenda Savings Card: limited to $25 per month for commercially insured patients with coverage, with low utilization given the broader generic liraglutide market. [11]
Application is straightforward in all cases: enter date of birth, prescription details, and insurance information at the manufacturer site, get a card or activation code, and present at the pharmacy. The pharmacy runs the card as a secondary claim after insurance, and you pay the residual.
Manufacturer direct cash programs (the big shift)
The most consequential pricing change of the last two years has been the manufacturers cutting out the middlemen and selling directly to self-pay patients at sharply lower prices through their own pharmacy operations. These channels exist primarily to keep cash patients from defecting to compounding pharmacies and grey-market international suppliers. [2][4][7]
NovoCare Pharmacy (Novo Nordisk)
NovoCare Pharmacy sells Wegovy directly to cash payers at $499 per month for all dose strengths from 0.25 mg through 2.4 mg, with the price the same regardless of whether you are titrating up or maintaining. The medication ships from the contracted Right Source mail-order pharmacy after a valid prescription is on file. NovoCare also runs the Ozempic self-pay program: $199 per month for the first two fills of 0.25 mg or 0.5 mg for new patients (offer valid through June 30, 2026), then $349 per month for 0.25, 0.5, or 1 mg, and $499 per month for 2 mg. The oral Rybelsus equivalent runs $149 per month for 1.5 mg and 4 mg starter doses, with higher-dose pricing in the $199 to $399 range. [6][7]
LillyDirect (Eli Lilly)
LillyDirect sells Zepbound vials (not pens) at four standard cash price points tied to dose: $349 for the 2.5 mg starter dose, $499 for 5 mg, $599 for 7.5 mg, and $699 for 10 mg. As of late 2025, LillyDirect added 12.5 mg vials at $849 and 15 mg vials at $1,049, finally giving cash patients access to the full dose range. The Self-Pay Journey Program lowers prices further for patients who refill on time: $299 for 2.5 mg, $399 for 5 mg, and $449 per month for all higher doses including 12.5 mg and 15 mg. To stay in the discounted Self-Pay Journey tier, you must complete each refill within 45 days of the previous delivery. LillyDirect partnered with Walmart Pharmacy in October 2025 to add retail pick-up of the same direct-to-consumer pricing in addition to mail order. [4][9][28]
What you actually need to use these
These programs require a real prescription from a licensed clinician. They are not coupons applied at a normal pharmacy; the medication ships through a specific contracted pharmacy or pickup point. Expect identity verification, a credit card on file, and a prescriber-driven enrollment. You cannot use a NovoCare or LillyDirect direct cash price simultaneously with insurance coverage; pick one or the other for a given fill.
Patient assistance programs (income-based, free or near-free)
For low-income patients with no insurance, both manufacturers run formal patient assistance programs that can provide medication at no cost when income and citizenship requirements are met. These are separate from the savings cards, are application-based, and take three to six weeks for first approval. [29][30]
Novo Nordisk Patient Assistance Program (NNPAP)
NNPAP covers Ozempic, Wegovy, Rybelsus, Victoza, Saxenda, and Novo's insulins. Income limit for Ozempic specifically is at or below 200 percent of the federal poverty level, as of the 2026 program update. For all other Novo products including Wegovy, the limit is at or below 400 percent of the federal poverty level. Patients must be uninsured or have inadequate insurance, US citizens or legal residents, and have a clinician complete the prescriber portion of the application. Approved patients receive medication directly from the program for up to 12 months at a time before reapplication. [29]
Lilly Cares Foundation
Lilly Cares covers Mounjaro, Zepbound, Trulicity, and Lilly's other branded medications. Income limits for 2026 are tiered by drug group: 300 percent of federal poverty level for Group 1 medications, 400 percent for Group 2, and 500 percent for Groups 3 and 4. For a one-person household in 2026, those translate to roughly $46,950, $62,600, and $78,250 respectively. Mounjaro and Zepbound are typically Group 3 or 4. Same uninsured / underinsured / citizenship requirements as NNPAP. Approved patients get medication shipped to their prescriber's office or directly to home for up to 12 months. [30]
| Program | Drugs covered | Income limit (1-person household, 2026) | Documentation |
|---|---|---|---|
| NNPAP (Novo Nordisk) | Ozempic, Wegovy, Rybelsus, Victoza, Saxenda | 200% FPL ($31,300) for Ozempic; 400% FPL ($62,600) for others | Prescriber form, proof of income, ID |
| Lilly Cares | Mounjaro, Zepbound, Trulicity | 500% FPL ($78,250) for Mounjaro / Zepbound | Prescriber form, proof of income, ID, US residency |
| PAN Foundation Obesity Fund | FDA-approved obesity drugs | Variable; insurance required (payor of last resort) | Up to $1,000 per year copay help [31] |
| HealthWell Foundation | Diabetes (when fund is open) | Up to 500% FPL when fund is open | Insurance required, fund availability varies |
| Patient Advocate Foundation | Various disease funds | Varies by fund | Merging with PAN as TotalAssist July 2026 [31] |
If you are between the patient assistance income cutoffs and the manufacturer cash price, the gap can sometimes be bridged by the PAN Foundation obesity copay fund (up to $1,000 per year, payor of last resort, requires insurance) or by stacking a state-specific assistance program with the manufacturer cash channel.
Compounded GLP-1 telehealth (the other low-cost path)
During the FDA shortage of semaglutide and tirzepatide that ran from 2022 through early 2025, 503A compounding pharmacies were permitted to prepare patient-specific compounded versions of these molecules for any clinically appropriate patient. A large telehealth industry grew up around this. Typical 2026 pricing: roughly $99 to $400 per month for compounded semaglutide and $125 to $600 per month for compounded tirzepatide, often bundled with the telehealth visit, dosing changes, and clinician support. [3][12][32]
The regulatory situation tightened sharply in 2025. The FDA declared the tirzepatide shortage resolved in October 2024 and the semaglutide shortage resolved in February 2025. Mass commercial compounding of essentially copies of the brand drugs is no longer permitted under the shortage exemption. 503A pharmacies can still prepare patient-specific compounds when there is a documented clinical need that the commercial product cannot meet, for example an allergy to an inactive ingredient or a specific dose not commercially available. The legal interpretation of what qualifies as a meaningful clinical difference is contested, and FDA enforcement is ongoing. Hims and Hers stopped offering compounded tirzepatide in March 2026 after a settlement with Novo Nordisk; Eli Lilly has pursued similar litigation. [32][33]
What you actually pay through telehealth in 2026
| Provider | Compounded semaglutide | Compounded tirzepatide | Notes |
|---|---|---|---|
| Trimi Health | ~$99 / mo (annual billing) | ~$125 / mo (annual billing) | 503A patient-specific [12] |
| Henry Meds | ~$179 / mo flat | ~$179 / mo flat | Includes clinician and pharmacy [12] |
| Mochi Health | ~$229 / mo + $79 membership | ~$229 / mo + $79 membership | Membership covers clinician [12] |
| Hims (semaglutide only post-2026 settlement) | ~$199 / mo | No longer offered | Settlement with Novo limits scope [32] |
| Ro | ~$199 / mo | $199 to $349 / mo by tier | Body program, telehealth-led [32] |
| LifeMD | Brand-name routing (Wegovy / Zepbound) | Brand-name routing | Pivoted away from compounded after enforcement |
If you are considering a compounded GLP-1 through telehealth, the difference between a legitimate operation and a risky one comes down to a few specifics:
- You are evaluated by a US-licensed clinician (MD, DO, NP, or PA) who reviews medical history and contraindications, not just an asynchronous form with no follow-up.
- The medication is dispensed by a state-licensed 503A pharmacy whose name and license number you can verify with the relevant state board of pharmacy.
- The pharmacy uses pharmaceutical-grade active pharmaceutical ingredient (API) sourced from an FDA-registered facility, with a Certificate of Analysis available on request.
- Pricing is transparent up front, including the cost of needles, sharps disposal, and any subscription fees beyond the medication itself.
- The provider has a written policy for documenting the patient-specific clinical need that justifies compounding under post-shortage rules.
Hard red flags: any "research only" or "not for human use" peptide sold by a chemical supply company, any program with no live clinician evaluation, any pharmacy that will not name itself or share its license number, and any product that ships without batch testing documentation. The FDA has warned about adverse events from non-sterile or mislabeled compounded semaglutide. See our compounded vs brand guide for a deeper safety walkthrough. [33]
International pricing and importation
International prices for the same drugs are dramatically lower than US list prices and lower than US cash channels in most cases. This is the single clearest illustration of how distorted US pricing is, and it explains why a steady stream of US patients self-import from Canadian, Mexican, and European pharmacies despite the legal grey zone. [13][17][34]
| Drug | United States (list) | United Kingdom | Germany | Japan | Canada | Mexico |
|---|---|---|---|---|---|---|
| Ozempic | $997 / mo [6] | ~$94 / mo [17] | ~$94 / mo [17] | ~$169 / mo [17] | $200 to $450 / mo [34] | ~$200 / mo (informal market reports) |
| Wegovy | $1,349 / mo [2] | £150 to £300 / mo [17] | ~$328 / mo [17] | Not yet broadly available | ~$400 / mo [34] | Variable |
| Mounjaro | $1,069 / mo [3] | £165 to £250 / mo | ~$444 / mo [17] | ~$319 / mo [17] | $300 to $550 / mo [34] | Variable |
The legal status of personal-use importation is constrained. The FDA's published policy is that personal importation of unapproved drugs is technically illegal but the agency exercises enforcement discretion for small quantities (typically defined as a 90-day supply or less) of non-controlled prescription drugs intended for personal use, particularly for serious conditions and when no US alternative is reasonably available. None of those conditions cleanly applies to GLP-1s now that domestic cash channels exist. Customs and Border Protection routinely seizes drug shipments from non-US pharmacies. Reliable cold-chain shipping for an injectable across borders is also a practical challenge: GLP-1 pens lose potency outside the 36 to 46 degree Fahrenheit range. We do not recommend international importation as a primary strategy, but it is worth knowing how distorted the US pricing context actually is. [13]
Most-Favored-Nation pricing and TrumpRx
In November 2025 the White House announced agreements with Eli Lilly and Novo Nordisk to apply Most-Favored-Nation (MFN) pricing to certain GLP-1s through a new direct-to-consumer government platform called TrumpRx, with parallel commitments for Medicare and Medicaid. The headline numbers: vials of GLP-1s indicated for weight management will be sold to consumers via TrumpRx at an average of $350 per month. Future FDA-approved oral GLP-1 starter doses (Lilly's orforglipron, Novo's Wegovy oral) are slated for $150 per month from either manufacturer on TrumpRx. Medicare and Medicaid will pay $245 per month net, with Medicare patient copay set at $50 (this is the financing behind the GLP-1 Bridge program). [16][22]
TrumpRx itself is scheduled to launch in early 2026, with Medicare coverage expansion phased in by 2027. As of mid-2026, the platform is operational for some products with limited GLP-1 availability and rolling expansion. The deal does not directly help a cash-pay patient under 65 with employer coverage that excludes weight-loss drugs, but it explains why Lilly added the Self-Pay Journey Program tiers and Novo expanded NovoCare Wegovy pricing simultaneously: both manufacturers are racing to retain direct relationships with cash patients before federal channels capture them at the negotiated price. [16][22]
Discount cards and big-box pharmacy bundles
GoodRx, SingleCare, and similar discount cards can shave a few hundred dollars off the retail brand price at chain pharmacies. As of mid-2026, GoodRx Saxenda coupons drop the price from a $1,472 average retail to about $372, and GoodRx liraglutide generic coupons land around $250 to $400. For Ozempic, Wegovy, Mounjaro, and Zepbound, GoodRx coupons rarely beat the manufacturer direct cash channels (NovoCare $499 Wegovy, LillyDirect $349 Zepbound), so GoodRx is most useful for patients who absolutely need a specific dose tier the manufacturer programs do not cover. Discount cards cannot be combined with insurance for the same fill, and they cannot be combined with manufacturer savings cards either. [11][35]
Costco, Sam's Club, and Amazon Pharmacy negotiate independent cash bundles for some GLP-1s, but again these typically run higher than the manufacturer direct programs for the FDA-approved indications. They can be useful for diabetes patients picking up Ozempic when the manufacturer card is exhausted or for filling smaller pen quantities.
Hidden costs people forget to budget for
The headline drug price is rarely the full cost of being on a GLP-1. A realistic monthly budget includes:
- Provider visits: initial telehealth or in-person consult $50 to $300, follow-ups every 4 to 12 weeks at $25 to $150 each. Some telehealth bundles include this; many do not.
- Lab work: baseline metabolic panel, A1c, lipid panel, sometimes thyroid and pregnancy testing. With insurance most of this is preventive-covered. Cash labs run $50 to $200 every 3 to 6 months.
- Needles and syringes: for vial-based programs (LillyDirect Zepbound vials, compounded), you supply your own. Insulin syringes run $0.20 to $0.50 each, so $6 to $15 a month.
- Sharps disposal: a 1-quart sharps container runs $5 to $15 and lasts 6 to 12 months. Mail-back disposal services run $20 to $50 per container.
- Cold storage and shipping: if you order through telehealth or direct-to-consumer, your medication ships overnight on ice. Most providers include this in the price; a few add a $25 to $50 shipping fee.
- Anti-nausea and side-effect management: Zofran, Imodium, fiber supplements, electrolyte tabs. Often $10 to $30 a month during titration.
- Time off work for clinical visits or side-effect days: not a line item, but real for many patients.
The all-in monthly cost of being on a GLP-1, even on the cheapest legal compounded path, is therefore typically $200 to $500 once you add everything beyond the headline drug price. For brand-name through manufacturer cash channels, $550 to $750 all-in is realistic.
Recent and upcoming price changes to watch
- NovoCare Wegovy expansion: Novo expanded the $499 NovoCare price to all dose strengths including the new HD 7.2 mg in early 2026, having previously charged more for higher doses.
- LillyDirect Zepbound full dose range: 12.5 mg and 15 mg vials added in late 2025, with the Self-Pay Journey Program flattening the higher-dose price to $449.
- Walmart Pharmacy LillyDirect pickup: launched October 2025, removing the mail-only constraint for Zepbound vials.
- Rybelsus list price cut: Novo announced February 2026 that 7 mg and 14 mg Rybelsus list price drops to $675 effective January 1, 2027.
- Medicare GLP-1 Bridge program: launches July 1, 2026, runs through December 31, 2027, $50 monthly copay for eligible Wegovy, Zepbound KwikPen, and Foundayo prescriptions. [22]
- BALANCE Model in Medicaid: rolling state opt-in starting May 2026, manufacturer participation required for negotiated pricing. [25]
- TrumpRx direct-to-consumer platform: early 2026 launch, $350 average for vials, $150 for future oral starter doses. [16]
- Generic liraglutide expansion: Hikma and Meitheal generic liraglutide on the market since late 2024 / early 2025, prices in the $250 to $500 range for cash payers, gradually displacing brand Victoza and offering a Saxenda alternative. [11]
- Patent cliff timing: Novo Nordisk's core semaglutide composition patents expire in late 2031 in the US. Generic semaglutide (likely from Hikma, Teva, and others) is expected to compress US pricing toward European levels in 2032 and after. Tirzepatide composition patents extend into the mid-2030s.
- PAN Foundation merger: PAN and Patient Advocate Foundation launch the unified TotalAssist program July 1, 2026, simplifying obesity copay applications. [31]
A practical decision framework
Use this as a starting point. Your specific plan, prescriber, and dose may shift the answer.
- Type 2 diabetes with any insurance: ask your prescriber to run a formulary check on Ozempic and Mounjaro. Add the manufacturer savings card (Ozempic or Mounjaro) on top. Most insured diabetes patients land at $25 to $100 per month all-in.
- Weight management with commercial insurance that covers the drug: add the Wegovy or Zepbound savings card. Most patients land at $25 per month with the card if their plan covers the drug.
- Weight management with commercial insurance that excludes the drug: NovoCare Pharmacy at $499 monthly for Wegovy, or LillyDirect Self-Pay Journey Program at $299 to $449 monthly for Zepbound vials, are the cleanest brand paths. The Mounjaro $573 cash savings offer or Zepbound $650 pen savings offer apply if you specifically need pens.
- Medicare Part D enrollee with type 2 diabetes: standard Part D coverage of Ozempic, Mounjaro, Trulicity, Rybelsus applies. The IRA $2,100 annual out-of-pocket cap is your ceiling. You cannot use the manufacturer savings cards.
- Medicare Part D enrollee with established CV disease and obesity: Wegovy is covered under standard Part D for the cardiovascular indication.
- Medicare Part D enrollee with obstructive sleep apnea and obesity: Zepbound is covered under standard Part D for the OSA indication.
- Medicare Part D enrollee with obesity plus a comorbidity, no qualifying indication: apply for the Medicare GLP-1 Bridge starting July 2026, $50 monthly copay for Wegovy, Zepbound KwikPen, or Foundayo.
- Medicaid enrollee: diabetes coverage is universal across all states. Obesity coverage exists in 13 states and is shrinking. Check your state Medicaid formulary directly. The CMS BALANCE Model may add coverage in your state from May 2026 onward.
- VA / TRICARE Prime / Select: diabetes GLP-1s covered with prior authorization. Weight-loss GLP-1s covered with PA on TRICARE Prime / Select, but not on TRICARE For Life since August 2025.
- Income-qualified, uninsured: apply to NNPAP (Novo) for Wegovy, Ozempic, Saxenda, or Rybelsus, or to Lilly Cares for Mounjaro or Zepbound. Approval typically takes 3 to 6 weeks; medication arrives free for up to 12 months.
- Off-label weight loss, tight budget, willing to accept non-FDA-approved formulation: a licensed telehealth provider working with a verified 503A compounding pharmacy currently sits in the $99 to $400 monthly range for compounded semaglutide and $125 to $600 for compounded tirzepatide. The trade-off is regulatory uncertainty and somewhat less consistent quality assurance than the brand product. See the compounded vs brand guide.
- Cash-pay older adult with cash savings willing to import: not recommended given existing US channels, but Canadian and UK pharmacy prices are typically 50 to 80 percent lower for the same product.
Whatever path you choose, the prescription should follow a real clinical evaluation, you should know the name and license number of the dispensing pharmacy, and the price you are quoted should be the price you are billed. If a program asks you to pay before sharing those details, it is not a legitimate program.
References
- Universal Drugstore. "Cheapest GLP-1 Options Online Without Insurance: A Complete Price Guide." universaldrugstore.com
- Novo Nordisk. "Novo Nordisk introduces NovoCare Pharmacy, lowering cost of all doses of FDA-approved Wegovy to $499 per month." PR Newswire. prnewswire.com
- Doctronic. "GLP-1 Cost Without Insurance: Price Comparison Chart." doctronic.ai
- Eli Lilly & Co. "Lilly launches additional Zepbound vial doses and offers new savings for self-pay patients." Investor release. investor.lilly.com
- Centers for Medicare & Medicaid Services. "Medicare GLP-1 Bridge." cms.gov
- Novo Nordisk. "Ozempic List Price & Insurance Coverage Explained." NovoCare. novocare.com
- Novo Nordisk. "Wegovy Cost, Coverage & Savings Resources." NovoCare. novocare.com
- Eli Lilly & Co. "Mounjaro Savings & Resources." mounjaro.lilly.com
- Eli Lilly & Co. "Zepbound Coverage, Affordability, and Savings." zepbound.lilly.com
- Novo Nordisk. "Rybelsus List Price & Insurance Coverage Explained." NovoCare. novocare.com
- GoodRx. "Liraglutide (Saxenda / Victoza) 2026 Prices, Coupons & Savings Tips." goodrx.com
- Trimi Health. "Cheapest Tirzepatide Providers 2026: All Options Ranked by Price." trytrimi.com
- Levi J, Wang J, Venter F, Hill A. "Estimated minimum prices and lowest available national prices for antiobesity medications." JAMA Network Open. 2023. jamanetwork.com
- Centers for Medicare & Medicaid Services. "Medicare Drug Price Negotiation Program." cms.gov
- Kaiser Family Foundation. "An Overview of Medicare Coverage and Spending on GLP-1s." kff.org
- Academy of Managed Care Pharmacy. "Federal Update: Trump Administration Announces Deal to Bring Most-Favored-Nation Pricing to GLP-1s." amcp.org
- Peterson-KFF Health System Tracker. "How do prices of drugs for weight loss in the U.S. compare to peer nations' prices?" healthsystemtracker.org
- GoodRx Research. "Tracking Insurance Coverage of Weight Loss Medications." goodrx.com
- Healthline. "GLP-1 Insurance Coverage for Weight Loss: 2026 Guide." healthline.com
- Wellcare. "Does Medicare Cover Weight-Loss Drugs? Understanding GLP-1 Coverage in 2026." wellcare.com
- U.S. News & World Report. "Medicare GLP-1 Coverage 2026: Ozempic, Zepbound & Costs." health.usnews.com
- NPR. "Medicare to launch weight loss drug option in July with $50 copay." npr.org
- Kaiser Family Foundation. "Medicaid Coverage of and Spending on GLP-1s." kff.org
- Stateline. "More states consider dropping GLP-1 weight loss drugs from Medicaid." stateline.org
- Centers for Medicare & Medicaid Services. "BALANCE Model: Better Approaches to Lifestyle and Nutrition for Comprehensive Health." cms.gov
- Military.com. "A VA Clinic Gave Veterans GLP-1s for Weight Loss. A Year Later, Everything Improved." military.com
- TRICARE / Express Scripts. "GLP-1 Medications (Diabetes and Weight Management)." militaryrx.express-scripts.com
- Walmart Corporate. "LillyDirect and Walmart Pharmacy Launch First Retail Pick-Up Option With Direct-to-Consumer Pricing for Zepbound." corporate.walmart.com
- Novo Nordisk. "Patient Assistance Program (NNPAP)." novocare.com
- Lilly Cares Foundation. "How to Apply." lillycares.com
- PAN Foundation. "PAN opens first obesity copay fund to expand access to treatment." panfoundation.org
- U.S. News & World Report. "How to Get GLP-1 Drugs Without Insurance." health.usnews.com
- U.S. Food & Drug Administration. "Medications Containing Semaglutide Marketed for Type 2 Diabetes or Weight Loss." fda.gov
- GLP1Prices Canada. "Ozempic Price Canada 2026: Compare 33+ Pharmacies." glp1prices.ca
- GoodRx. "GLP-1 Drug Savings: A Complete Guide for How to Save on Ozempic, Wegovy, and More." goodrx.com