GLP-1 Injection Guide
Summary: GLP-1 medications are given as a small subcutaneous injection in the abdomen, thigh, or upper arm using either a prefilled pen or a vial and insulin syringe. This guide walks through pen priming, vial draw-up, injection technique, storage rules per brand, site rotation, travel, troubleshooting, and what to do when something feels off.
This content is for informational purposes only and is not medical advice. Always consult a qualified healthcare provider before starting, changing, or stopping any medication.
Pens vs vial-and-syringe: what you'll be using
Brand-name GLP-1 medications come as prefilled pens. Ozempic (semaglutide for type 2 diabetes) uses a multi-dose dial pen that holds four weekly doses; Wegovy (semaglutide for weight management) uses a single-dose disposable pen with no dial; Mounjaro and Zepbound (tirzepatide, made by Eli Lilly) use single-dose auto-injectors that release the medication when you press them against the skin; and Saxenda and Victoza (liraglutide, given daily) use multi-dose dial pens similar in form to the Ozempic device. [1][2][3][4][5] Compounded semaglutide and tirzepatide from a 503A or 503B pharmacy almost always arrive as a multi-dose vial that you draw up with a small insulin syringe, typically a U-100 0.3 mL or 0.5 mL syringe with a 29 to 31 gauge needle. Zepbound vials supplied through LillyDirect are single-use vials that you draw with a separate 1 mL syringe and needle. [6]

The drug ends up in the same place either way: just under the skin, into the fatty tissue. The technique differs mostly in how you measure the dose. With a pen, the device counts it for you. With a vial, you read the markings on the syringe barrel yourself, which means the prescriber should give you a dose written in both milligrams and units (or milliliters) of the specific concentration you were dispensed. [7] Compounded products in particular vary by concentration, and the same prescribed milligram dose can mean a very different number of units depending on whether the vial is labeled 2.5 mg/mL, 5 mg/mL, or 10 mg/mL. [8]
Storage rules by brand
Unopened pens and unopened vials live in the refrigerator at 36 to 46 degrees F (2 to 8 degrees C) until first use, kept in the original carton to protect them from light. Never freeze a GLP-1 medication; if it has frozen, throw it out. [1][9] Once a pen or vial is in use, the in-use stability varies by brand, and confusing the rules is one of the most common ways patients waste medication.
- Ozempic pen (semaglutide). Store unopened in the refrigerator. Once in use, keep in the refrigerator or at room temperature between 59 and 86 degrees F (15 and 30 degrees C) for up to 56 days, then discard whatever remains. [1][9]
- Wegovy pen (semaglutide). Store unopened in the refrigerator. If refrigeration is not available, unopened pens may sit at temperatures up to 86 degrees F (30 degrees C) for up to 28 days. Each pen is single-use, so the in-use clock applies only between when you take it out and when you inject it. [2][10]
- Mounjaro pen (tirzepatide). Refrigerated storage. Once removed for use, may be kept below 86 degrees F (30 degrees C) for up to 21 days, then discard if unused. [3]
- Zepbound auto-injector pen (tirzepatide). Same as Mounjaro: refrigerated, with up to 21 days at room temperature. [4]
- Zepbound single-dose vials (LillyDirect). Store all unopened vials refrigerated. Vials may be kept at room temperature up to 86 degrees F (30 degrees C) for up to 21 days. Each vial is intended for a single dose, so partial vials should not be saved. [6]
- Saxenda pen (liraglutide). Refrigerated until first use. Once in use, may be stored in the refrigerator or at room temperature between 59 and 86 degrees F (15 and 30 degrees C) for up to 30 days, then discarded even if medication remains. [5]
- Victoza pen (liraglutide). Same in-use rule as Saxenda: 30 days at room temperature or refrigerated after first use.
- Compounded vials. Follow the dating from the dispensing pharmacy, usually 28 to 90 days refrigerated after first puncture. Beyond-use dates printed on the label are pharmacy-specific and should be treated as hard expirations.
Letting a refrigerated pen or syringe warm to room temperature for 15 to 30 minutes before injecting reduces stinging on entry. [1] Cold medication is also more viscous, which makes the plunger harder to press on a vial draw and can stretch the held injection time on a pen.
Pre-injection checklist
Before every dose, run through the same short checklist. It takes a minute and prevents most user errors.
- Wash your hands with soap and water and dry them.
- Confirm the medication name, strength, lot number, and expiration date on the label.
- Inspect the liquid through the pen window or vial: it should be clear and colorless to slightly yellow. Cloudiness, particles, suspended flakes, or a brown or pink tint mean do not use. [1][11]
- Let the pen or syringe sit out 15 to 30 minutes to reach room temperature. Do not microwave, soak in warm water, or place near a heat source.
- Gather supplies: alcohol swab, new pen needle or insulin syringe, sharps container within arm's reach, bandage in case of bleeding, and a small adhesive site sticker if you are tracking rotation.
- Pick a clean, dry injection site. Wipe it with the alcohol swab and let it air dry; injecting through wet alcohol stings.
Where to inject: sites, rotation, and lipohypertrophy
All FDA-approved GLP-1 medications can go into one of three areas: the abdomen, the front of the thigh, or the back of the upper arm. The upper arm is hard to reach yourself and is usually used when a partner or caregiver is doing the injection. [1][2][12]
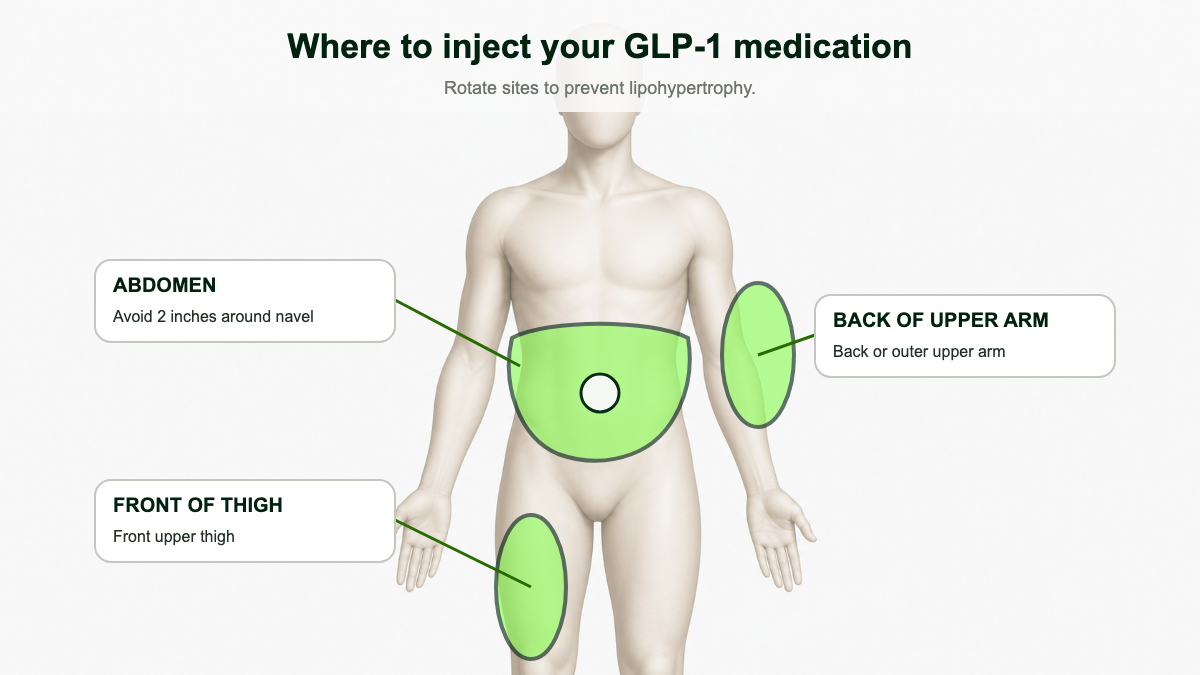
- Abdomen. Stay at least 2 inches away from the navel in any direction. Avoid the waistband area where clothing rubs. Most users find the abdomen the easiest site because the subcutaneous layer is thicker and easier to pinch, and absorption is consistent. [12]
- Thigh. Use the front and outer portion of the upper thigh, roughly the middle third between the hip and knee. Avoid the inner thigh, the area directly over the knee, and any spot directly over muscle.
- Upper arm. Back and outer side, in the fatty area behind the triceps. This site is generally only practical with a helper.
Rotate sites with each dose. A simple weekly pattern is left abdomen, right abdomen, left thigh, right thigh, then repeat. For daily medications such as Saxenda and Victoza, rotation matters even more because you are injecting seven times more often; a common pattern is to map the abdomen as a four-by-four grid and step through the squares one per day, leaving each individual spot at least two weeks of rest. [13]
Repeated injections into the same small spot can cause lipohypertrophy, a firm fatty lump under the skin that absorbs medication unpredictably. The lump may feel rubbery or dense, look slightly raised, and have less sensation than surrounding tissue. Once it forms, the area should be avoided for several months while it heals. Correct rotation is the single most effective way to prevent it; using a fresh needle for each injection also matters because reused needles develop microscopic burrs that traumatize tissue. [13] Avoid skin that is bruised, scarred, irritated, tattooed, infected, or near a mole. The injection site does not change how the drug works or how much weight you lose. [12]
Step-by-step: Ozempic multi-dose dial pen
The Ozempic pen holds four weekly doses and is dialed each time. Rybelsus is an oral form of semaglutide and is not injected, so it does not appear in this section.
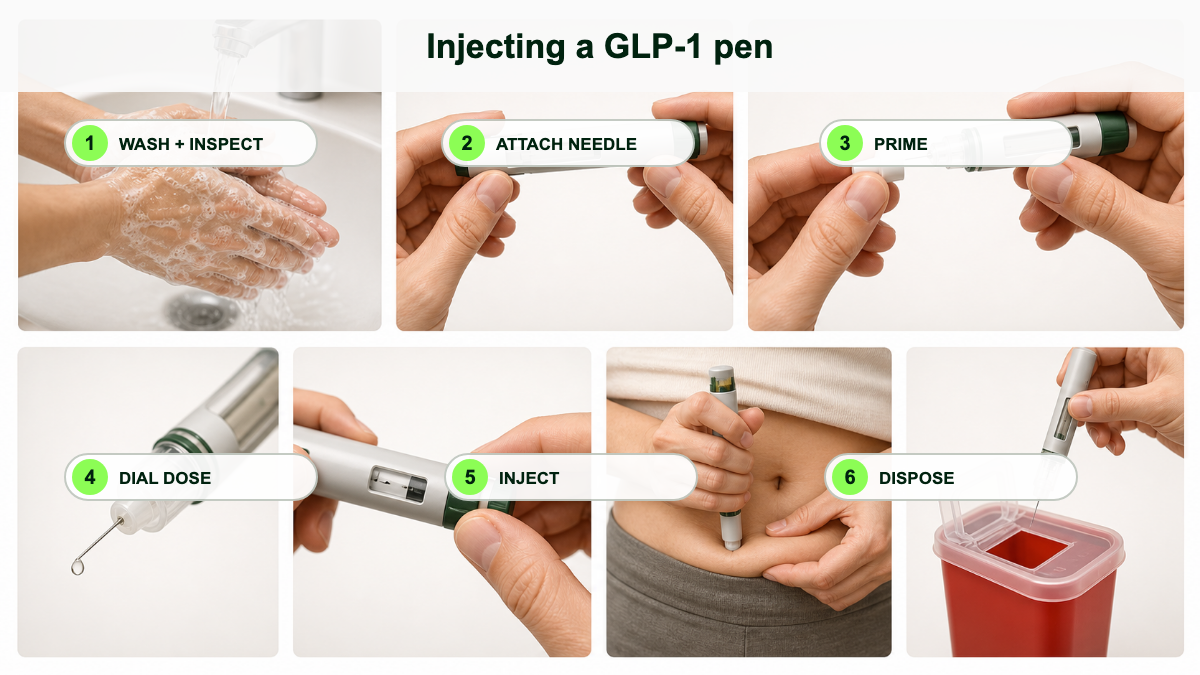
- Pull off the pen cap. Wipe the rubber seal at the tip with an alcohol swab.
- Tear the paper tab off a new pen needle and screw it straight onto the pen until snug. Pull off the outer needle cap (save it for disposal) and the inner needle cap (throw it away).
- Flow check (only on a brand-new pen). Turn the dose selector to the flow-check symbol. Hold the pen with the needle pointing up, tap the cartridge gently, then press and hold the dose button until the counter returns to 0. A drop of liquid should appear at the needle tip. If no drop appears, repeat the flow check up to six times. If still nothing, change the needle and try once more. If a drop never appears, the pen is defective. [1][9][14]
- Turn the dose selector until the dose counter shows your prescribed dose (for Ozempic: 0.25, 0.5, 1, or 2 mg). The dial clicks as it turns. If you turn past your dose, simply turn back; no medication is wasted.
- Insert the needle straight into your skin at a 90-degree angle. You can pinch a fold of skin if you are very lean.
- Press and hold the dose button. When the counter reads 0, keep the button pressed and slowly count to 6 before pulling the needle out. This count makes sure the full dose is delivered. [1][9][11]
- Slide the outer needle cap back over the needle on a flat surface using the one-handed scoop, unscrew the needle, and drop it into your sharps container. Replace the pen cap and put the pen back into storage.
Step-by-step: Wegovy single-dose pen
Wegovy uses a different device. Each pen is preset to one weekly dose at the factory (0.25, 0.5, 1.0, 1.7, or 2.4 mg) and is discarded after a single use. There is no dial and no separate needle to attach; the needle is hidden inside the pen and exposed only when you press it against the skin. [10][15]
- Take the pen out of the refrigerator and inspect the window: the liquid should be clear and colorless. Verify the dose printed on the label matches what was prescribed.
- Wash your hands. Wipe your chosen injection site with an alcohol swab and let it dry.
- Pull the pen cap straight off. Do not put it back on; doing so could damage the needle.
- Place the pen flat against your skin so the needle guard is fully in contact and the pen is at a 90-degree angle.
- Push the pen firmly into your skin until you hear the first click. The yellow bar in the inspection window will start to move, signaling that the injection has begun. [15]
- Keep pressing the pen firmly against the skin. You may hear a second click during the injection; this is normal and means the dose is still being delivered.
- Continue holding the pen against the skin for about 10 seconds until the yellow bar has fully stopped moving. Lifting too early can interrupt the dose. [15]
- Slowly lift the pen straight up off the skin. The needle guard will lock over the needle. Drop the entire used pen into your sharps container.
Step-by-step: Mounjaro and Zepbound auto-injector
The Lilly tirzepatide pens are pre-loaded with one full dose. There is nothing to dial and no needle to attach. The needle retracts automatically after the injection. [3][4]
- Take the pen out of the refrigerator and let it warm at room temperature for at least 30 minutes.
- Check the label and the inspection window: liquid should be clear and colorless to slightly yellow.
- Wash your hands. Wipe the chosen site with an alcohol swab and let it dry.
- Pull the gray base cap off only when you are ready to inject. Do not touch the clear base; touching it can trigger a misfire.
- Place the clear base flat against the skin so the entire base is in contact. The pen will not fire unless it is pressed firmly.
- Press and hold the purple injection button. You will hear a first click as the injection starts.
- Continue holding the pen against the skin for about 10 seconds until you hear a second click and the gray plunger is fully visible in the window. Then lift the pen straight off. [3]
- Drop the entire used pen into your sharps container. The needle retracts automatically.
Step-by-step: Saxenda and Victoza daily pen
Saxenda and Victoza use the same multi-dose pen platform as Ozempic but are taken once daily rather than weekly. Because the pen is used so much more often, attention to site rotation and needle disposal becomes especially important. [5][16]
- Wash your hands. Pull off the pen cap.
- Attach a new pen needle by pulling off the paper tab and screwing the needle straight onto the pen. Remove the outer and inner caps.
- Flow check on each new pen and any time the pen has been jolted or dropped. Dial 2 units, hold the pen with the needle up, and press the button until a drop appears. Repeat up to six times if needed.
- Dial your prescribed dose. Saxenda titrates from 0.6 mg up to 3.0 mg over five weeks; Victoza is dosed at 0.6, 1.2, or 1.8 mg.
- Pinch a fold of skin if you are lean and insert the needle at a 90-degree angle.
- Press and hold the dose button until the counter returns to 0, then keep the needle in place for an additional six-second count to make sure the full dose is delivered.
- Withdraw the needle, scoop-recap, unscrew, and dispose of the needle in your sharps container.
- Mark the site on a small calendar or log so the next day you can step at least 2 cm away.
Step-by-step: vial and insulin syringe (compounded and Zepbound vial)
This is the workflow most compounded semaglutide and tirzepatide users follow, and it also applies to the single-dose Zepbound vials supplied through LillyDirect (with the size of the syringe adjusted as your prescriber directs). Confirm with your prescriber exactly how many units of the specific concentration equal your dose; this is the most common source of compounding errors. [6][8]
- Wipe the rubber stopper of the vial with an alcohol swab.
- Remove the cap from a new insulin syringe. For most compounded GLP-1 vials this is a U-100 0.3 mL or 0.5 mL insulin syringe with a 29 to 31 gauge needle. Pull the plunger back to the unit mark equal to your prescribed dose to draw air into the syringe.
- Push the needle straight down through the rubber stopper and inject the air into the vial. This equalizes pressure and makes the liquid easier to draw.
- Turn the vial upside down with the syringe still inserted. Keep the needle tip below the liquid line.
- Slowly pull the plunger to the correct unit mark. If you see large air bubbles, push the liquid back in and re-draw, or tap the barrel and push the bubbles out until the meniscus sits exactly on your dose line. A few tiny bubbles are not dangerous in subcutaneous injection (this is not a vein), but accuracy matters because they displace medication.
- Remove the needle from the vial. Recap only with the original cap or, better, do not recap at all and proceed straight to the injection.
- Wipe the injection site with alcohol and let it dry. Pinch a small fold of skin between thumb and forefinger.
- Insert the needle in one quick motion. Use a 90-degree angle if you have more than 1 inch of pinchable subcutaneous tissue at the site, or a 45-degree angle if you are lean and have less than 1 inch of pinchable tissue. Short insulin needles (4 to 6 mm) reach subcutaneous tissue safely at 90 degrees for nearly all body types. [17]
- Release the pinch. Push the plunger down steadily until it stops. Wait 5 to 10 seconds, then withdraw the needle straight out.
- Drop the entire syringe, needle attached, into the sharps container.
Dose calculation for compounded vials. The conversion is: units = (dose in mg / concentration in mg per mL) x 100. For a 5 mg/mL vial and a prescribed 0.5 mg dose, that is 0.5 / 5 x 100 = 10 units on a U-100 syringe. The same 0.5 mg dose drawn from a 2.5 mg/mL vial would be 20 units. Always re-derive the number when a new vial concentration is dispensed and confirm it with the pharmacy before injecting. [8]
Disposal: sharps containers and mail-back programs
Every used needle, pen needle, prefilled pen, and used vial goes into an FDA-cleared sharps container immediately after use. Do not recap needles before disposal except with the one-handed scoop technique used to transfer pen needles into the container. [18]
If you do not have a commercial sharps container, a heavy-duty plastic laundry detergent or bleach bottle with a screw lid works as a household substitute; label it clearly with "do not recycle" or "sharps" and never put it in regular recycling. [9] Most commercial containers are marked with a fill line at roughly three-quarters full, beyond which they should be sealed and disposed of.
Disposal options vary by state. Common routes include: drop-off at a participating pharmacy, hospital, or fire station; community sharps collection events; mail-back programs from companies such as Stericycle, PureWay, or the manufacturer's own program (Novo Nordisk offers a free disposal container through NovoCare for Ozempic, Wegovy, and Saxenda users); and household hazardous waste collection sites. [18][19] The website safeneedledisposal.org maintains a state-by-state locator. Never throw loose sharps into household trash or recycling, where they pose injury risk to sanitation workers.
For travel, a small portable sharps container or a hard-sided pencil case lined with the original needle caps works for short trips; transfer the contents to your full container at home.
Travel: TSA, cooling cases, and time zones
The TSA allows medically necessary liquids over 3.4 ounces in carry-on luggage, including injectable medications, ice packs, gel packs, and freezer packs needed to keep them cool, even if those packs are partially melted at screening. Declare them at the security checkpoint before your bags enter the X-ray. [20]
- Carry the medication in its original labeled box or pharmacy packaging with the prescription label visible.
- Bring a printed or digital copy of your prescription, especially for international travel.
- Pack pens and vials in your carry-on, never in checked baggage where the cargo hold can reach freezing temperatures and ruin the medication.
- Use an insulated cooling case for any travel longer than the in-use room-temperature window of your specific medication. FRIO evaporative cooling wallets activate by soaking in water for five to ten minutes and hold pens between 64 and 79 degrees F for up to 45 hours without electricity. Vivi Cap and MedAngel offer active electronic options.
- For time zones, the general rule is that small shifts (under three hours) do not require a dose adjustment for weekly medications; you can stay on your home schedule or shift to the new local time on your usual injection day. For larger shifts or for daily medications, ask your prescriber for guidance.
- For international travel, carry a doctor's letter listing the medication and the needles. Some countries (Japan, Singapore, UAE) require advance declarations for prescription injectables.
Common problems and fixes
A few situations come up often enough that they are worth planning for in advance.
- No drop at the flow check. Replace the needle and try the flow check again. If still no drop after six attempts on a new needle, the pen is defective and should be exchanged at the pharmacy. Novo Nordisk customer service (1-888-693-6742 in the U.S.) handles Ozempic, Wegovy, and Saxenda pen replacements; Lilly handles Mounjaro and Zepbound. [1][14]
- "No medication came out" after a normal-looking injection. Diagnose by checking the dose counter (it should read 0), the needle (look for a wet drop), and the skin (look for a small bead of liquid leakage). Some leakage at the surface is normal. If the counter never returned to 0, do not redose; contact your prescriber.
- Bent or damaged needle. Do not use it. Remove and replace with a fresh needle before injecting. A bent needle usually means the pen contacted a hard surface; check the cap and storage spot.
- Pen will not dial. Most often this means the pen is empty or has less than the dialed dose remaining. Check the cartridge window. If liquid is present but the dial sticks, the pen is defective. Do not force it.
- Bubbles in the cartridge or syringe. Small bubbles are cosmetic in subcutaneous injection. Large bubbles in a syringe should be cleared during draw-up by re-pushing the medication into the vial and re-drawing.
- Small drop of blood at the site. Normal. A tiny capillary was nicked. Apply gentle pressure with a clean tissue for 10 to 20 seconds. Do not rub. Bruising over the next day is also normal and unrelated to dose.
- Stinging during injection. Almost always caused by cold medication or wet alcohol. Let the pen warm 15 to 30 minutes and let alcohol dry fully before piercing. Smaller-gauge needles (32G is thinner than 30G) hurt less. [21]
- Pain that lasts more than a few hours, with redness or swelling. Possible site reaction or rare infection. Photograph it, mark the edge with a pen, and contact your prescriber if it spreads or worsens.
- Missed dose, semaglutide (Ozempic, Wegovy). If less than 5 days late, take it as soon as you remember. If more than 5 days late, skip it and take the next dose on your usual day. [1][9]
- Missed dose, tirzepatide (Mounjaro, Zepbound). If less than 4 days late, take it as soon as you remember. If more than 4 days late, skip it and resume on your regular day.
- Missed dose, liraglutide (Saxenda, Victoza). Skip the missed dose and take the next one at your normal time. Do not double up.
Pain reduction tips
Most users report that the injection becomes nearly unnoticeable after the first month. A few small adjustments make the early weeks easier.
- Warm the pen at room temperature for at least 15 to 30 minutes before injecting.
- Hold an ice cube wrapped in a paper towel against the skin for 30 seconds before piercing. This is the single most effective trick for needle-shy users.
- Let alcohol fully evaporate from the skin before insertion. Wet alcohol stings sharply.
- Use the smallest gauge needle compatible with your pen or syringe. For pens, 32G x 4mm or 32G x 5mm needles fit Novo Nordisk pens and are noticeably more comfortable than the 31G or 30G needles many pharmacies dispense by default. [21]
- Insert the needle in one fluid motion rather than pressing slowly. Slow insertion stimulates more pain receptors.
- Avoid very sensitive areas: any spot that feels tender to a normal touch is also more sensitive to the needle.
- Breathe out as the needle goes in; muscle tension increases perceived pain.
Special situations
Tattoos, scars, and skin conditions. Avoid injecting through tattoos, scars, stretch marks with raised tissue, moles, varicose veins, eczema patches, or any irritated skin. Pick a spot at least 1 inch away.
Pregnancy and breastfeeding. Do not continue GLP-1 medications during pregnancy. Wegovy and Saxenda labels specifically advise discontinuation at least 2 months before a planned pregnancy. If you discover you are pregnant while on a GLP-1, stop and contact your prescriber immediately.
Acute illness. Continue your normal schedule during a routine cold or short stomach bug. If vomiting prevents you from keeping fluids down for more than a few hours, contact your prescriber; severe vomiting can interfere with medication absorption indirectly through dehydration and is also a sign that the GLP-1 dose may need to be adjusted.
Surgery and procedures with anesthesia. GLP-1 medications slow gastric emptying, which can raise the risk of regurgitation under anesthesia. Recent multi-society guidance from the American Society of Anesthesiologists and gastroenterology and obesity medicine societies suggests that most patients can continue GLP-1 medications before elective surgery, but those with active GI symptoms (nausea, vomiting, abdominal pain, bloating) should delay until symptoms resolve. Some clinicians still advise holding weekly GLP-1s for one week and daily ones on the day of surgery, particularly for procedures involving the upper GI tract. Always disclose your GLP-1 use to your surgeon and anesthesiologist at least one week ahead. [22]
Using insulin alongside a GLP-1. If you take both, use different injection sites at the same session and ideally different time slots. Mixing insulin and GLP-1 in the same syringe is not approved. Many providers recommend rotating GLP-1 sites across the abdomen and using thighs for insulin, or vice versa, so that lipohypertrophy from one does not interfere with the other.
Children and adolescents. Wegovy is FDA-approved for adolescents 12 and older with obesity, and Saxenda is approved for adolescents 12 and older as well. The injection technique is identical to adult administration, but adult supervision is required for adolescents who are new to self-injection. Many families share the responsibility for the first month, with the parent inspecting the pen and site while the adolescent performs the injection. [23]
Building a sustainable weekly routine
Most users settle into a fixed weekly ritual within the first month. Picking a consistent day and time helps the body adjust to the gastrointestinal effects and makes missed doses less likely. Sunday evening or Monday morning are common choices for working adults because they tend to land on a calm part of the week and align side-effect peaks with familiar surroundings. For daily medications, anchoring the injection to an existing daily habit (morning coffee, brushing teeth at night) cuts down on missed doses dramatically.
A simple log helps. A paper sticker calendar, a notes app entry with the date, dose, and site, or a dedicated tracker app can all work. Three pieces of information are worth recording for every injection: the date, the site (left abdomen, right thigh, etc.), and any unusual reaction. Over months this log makes patterns visible that would otherwise be invisible: a particular site that bruises more often, a brand of needle that hurts less, or a dose increase that coincided with a side-effect change.
Plan your supply chain. A two-pen buffer in the refrigerator prevents the panic of a delayed pharmacy refill, and a small bag of pen needles, alcohol swabs, and bandages stored next to your medication keeps the entire routine in one place. If you travel often, a duplicate kit kept in a packed travel bag eliminates one item from the pre-trip checklist.
Final notes
The injection itself takes under 15 seconds once you are comfortable with the routine. Most people who started anxious report after a month or two that they barely feel it. The main mistakes that cause real problems are skipping the warm-up time, reusing needles, neglecting site rotation, and miscalculating doses on compounded vials. If you avoid those four, the rest of the routine becomes muscle memory.
If something about the injection feels off (the pen sounds different, the medication looks cloudy, the site reacts unusually, or the dose counter behaves unexpectedly), pause before injecting and call your prescriber or the manufacturer's patient support line. Skipping a single dose to clarify a question is far safer than injecting medication you are unsure of. Most pen problems have known fixes, and most injection-site concerns resolve on their own, but the cost of pausing to confirm is low and the cost of a wrong injection can be high.
References
- Novo Nordisk. Ozempic Pen User Guide and Dosing Instructions. ozempic.com/how-to-take/ozempic-pen.html
- Novo Nordisk. How to Use the Wegovy Pen. wegovy.com/taking-wegovy/how-to-use-the-wegovy-pen.html
- Eli Lilly. Mounjaro: How to Take Mounjaro (auto-injector instructions). mounjaro.lilly.com/how-to-take-mounjaro
- Eli Lilly. Zepbound: How to Use Zepbound. zepbound.lilly.com/weight/how-to-use
- Novo Nordisk. Saxenda Weight-Loss Pen Instructions. saxenda.com/about-saxenda/how-to-use-the-pen.html
- Eli Lilly. Zepbound Vial Instructions for Use (LillyDirect). pi.lilly.com/us/zepbound-vial-us-ifu.pdf
- U.S. Food and Drug Administration. Compounding and the FDA: Questions and Answers. fda.gov/drugs/human-drug-compounding
- SeekPeptides / Eden. Semaglutide Dosage in Units: Conversion Charts and Calculation. tryeden.com/post/semaglutide-dosage-in-units-chart
- Novo Nordisk / novoMEDLINK. Ozempic Administration: Storage, Pen Instructions, and Disposal. novomedlink.com/diabetes/products/treatments/ozempic/dosing-administration/administration/pen.html
- Novo Nordisk. Wegovy (semaglutide) Prescribing Information and Storage. wegovy.com
- Medical News Today. Ozempic: How to Inject. medicalnewstoday.com/articles/drugs-how-to-administer-ozempic
- Healthline. Tips and Sites for Injecting Ozempic. healthline.com/health/drugs/where-to-inject-ozempic
- Cleveland Clinic. Lipohypertrophy: Symptoms, Causes, Treatment, Prevention. my.clevelandclinic.org/health/diseases/22928-lipohypertrophy
- 4allfamily / TrimRX. Ozempic Pen Not Working: Malfunctions and Troubleshooting Steps. 4allfamily.com/blogs/diabetes/ozempic-pen-not-working-malfunctions-and-troubleshooting
- Wegovy. Wegovy Pen Guide: First Click, Yellow Bar, Second Click. wegovy.com/obesity/starting-wegovy/starting-wegovy-pen.html
- Novo Nordisk. Victoza Patient Information and Pen Instructions. victoza.com
- Lilly Medical. Tips for Subcutaneous Injection (angle and pinch technique). medical.lilly.com/us
- U.S. Food and Drug Administration. Sharps Disposal Containers. fda.gov/medical-devices/safely-using-sharps-needles-and-syringes-home-work-and-travel/sharps-disposal-containers
- Safe Needle Disposal. State-by-state sharps collection locator and mail-back programs. safeneedledisposal.org
- Transportation Security Administration. Traveling with Medication and Medically Necessary Liquids. tsa.gov/travel/special-procedures
- ADW Diabetes. Understanding Insulin Needle Gauges (29G to 32G). adwdiabetes.com/articles/understanding-insulin-needle-gauges-27g-vs-28g-vs-29g-vs-30g-vs-31g
- American Society of Anesthesiologists. Multi-Society Consensus Guidance on Preoperative Management of Patients on GLP-1 Receptor Agonists. asahq.org/about-asa/newsroom/news-releases/2024/10/new-multi-society-glp-1-guidance
- Novo Nordisk. Wegovy for Adolescents with Obesity. wegovy.com/about-wegovy/wegovy-for-adolescents.html